- Bewertung wird geladen...
Inguinal hernias (groin hernias) are one of the world's most common conditions. In Germany alone, more than new 250,000 inguinal hernias are operated on every year. Men in particular are affected by this condition, more so than women.
It is estimated that around 20% of men will experience an inguinal hernia at some point in their life. The ratio of cases in men to women is 9:1.
An inguinal hernia may be congenital or acquired.
The most common form of hernia is the congenital type (indirect inguinal hernia), with 49% of cases occurring on the right-hand side, 38% on the left-hand side and 13% occurring on both sides.
Congenital inguinal hernias develop as a result of incomplete development of the abdominal wall during foetal development.
An acquired hernia (direct inguinal hernia) develops due to weakness of the abdominal muscles in the groin region.
This can sometimes be caused by a constitutional or degenerative connective tissue weakness (collagen metabolism defect), obesity, age and smoking. Another possible cause of direct inguinal hernias is increased pressure inside the abdomen, for example due to prostate enlargement, pregnancy or chronic bronchitis.
Inguinal hernias are less common among women due to the anatomy of their groin area.
Symptoms: inguinal hernias can cause a variety of symptoms. Commonly, there is a bulging in the groin region, which can vary greatly in size. This can be pressed back in (reduced) when standing, but sometimes only when lying down.
Pain often only occurs after exertion, but frequently also happens while sitting and after prolonged periods of standing. This pain is caused by pressure on the nerves in the inguinal canal or by irritation of the peritoneum (hernial sac). The pain feels like a dragging sensation, can be stitch-like or burning, and occasionally radiates towards the testicles and the inside of the thigh.
A hernia becomes complicated and life-threatening if part of the intestine gets trapped in the hernial sac (Incarceration). The symptoms of this are excruciating pain in the groin and abdomen, as well as feeling seriously ill. The bulge can no longer be reduced when lying down, it becomes hard and the skin in the area becomes reddened.
The symptoms of sports hernia (Sports hernia) are similar to those of an inguinal hernia, although the cause of the pain with this condition is primarily nerve compression. Characteristically, the pain can temporarily be improved with rest, however as soon as the groin is put under strain again, the same symptoms recur.
Your doctor will only be able to determine which option is best for treating your inguinal hernia after a detailed examination.
Only once an accurate diagnosis has been made will your doctor draw up a meticulous plan for surgery with you and explain to you in detail what happens next.
Given that there are a great number of techniques and surgical methods available, your physical condition and past medical history will also be taken into consideration.
Of course, it also matters whether you are a professional athlete or just a "regular" sports player, since these facts can also help decide the most appropriate surgical technique.
The specialist can diagnose an inguinal hernia simply by asking specific questions about your medical history and performing a specific physical examination.
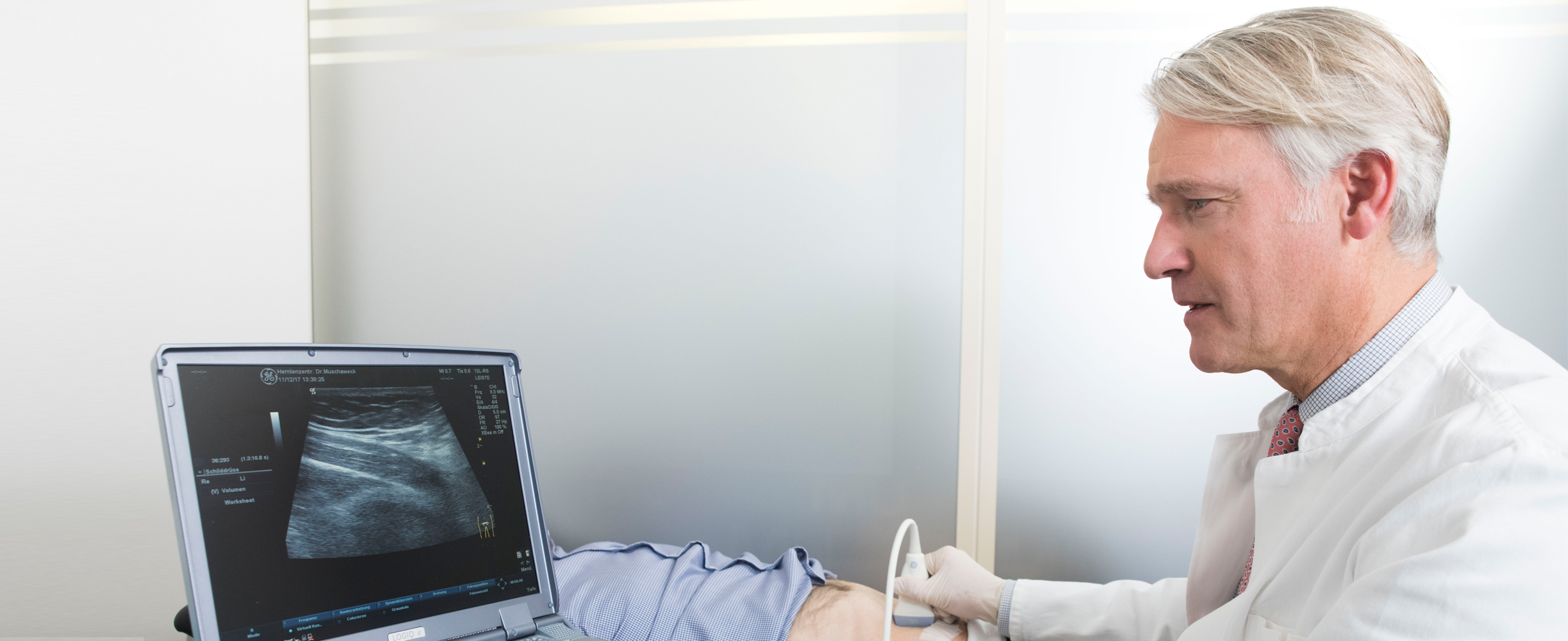
An ultrasound (sonography) examination carried out by an experienced practitioner can maximise the accuracy of the diagnosis. It also confirms the diagnosis in severely overweight patients, objectivises the findings and plays a key role in delineating and excluding other conditions (differential diagnoses).
This ensures that it is possible well in advance to plan a repair procedure that is tailored specifically to the patient's requirements.
An inguinal hernia can usually be diagnosed simply by clinical examination, i.e. following inspection and palpation of the hernial orifice. We also, as a rule, carry out an ultrasound examination of the groin region (static and dynamic ultrasound).
This allows the exact size of the hernial ring and hernial orifice to be determined, and an assessment of the contents of the hernial sac. It also allows other pathological changes to be ruled out (e.g. lymph node enlargement, cysts, vascular swellings such as aneurysms).
Further diagnostic procedures may be necessary in patients with recurrent hernias and/or chronic groin pain. Following the previous insertion of a mesh especially (open or laparoscopically), a CT scan or MRI scan of the abdomen may be useful for determining the cause of the problem.
With more persistent groin pain in particular, a neurological examination can be useful in getting to the root of the problem.
We would be delighted to advise you in more detail and give you more information about the treatment options and surgical options available for inguinal hernia repair. We will of course also explain to you in detail any possible risks and dangers associated with your procedure. All this will be explained to you again calmly during your pre-op consultation.